Periodontal diseases are infections of the gums that gradually destroy the support of your natural teeth. Patients over the age of 35 now lose more teeth to periodontal issues than any other cause.
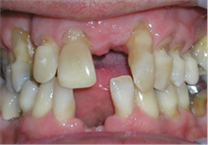
DETECTING PERIODONTAL DISEASE
Some warning signs of gum disease include:
- Bleeding gums
- Persistent bad breath
- Receding gums
- Changes in your bite
- Tooth movement
- Loosening and mobility of teeth
Dental plaque is the primary cause of gum disease in genetically-susceptible individuals. Bacteria found in plaque produce toxins or poisons that irritate the gums. They may cause them to turn red, swell, and bleed easily. If this irritation is prolonged, the gums separate from the teeth causing pockets (spaces) to form. Plaque can also harden into a rough, porous substance known as calculus (or tartar). This can occur both above and below the gum line.
As periodontal diseases progress, the supporting gum tissue and bone that holds teeth in place deteriorate. If left untreated, this leads to tooth loss. When your gums become unhealthy, they can become swollen and inflamed, bleed and recede. Mouth odor can come from this type of infection.
In later stages, the supporting bone is destroyed and your teeth will shift, loosen, or become painful and removal is then required. These changes not only affect your ability to chew and speak. They also spoil your smile.
However, don’t be fooled if these typical symptoms do not show up. With periodontal disease, bleeding, redness, and swelling are not always obvious. Further, pain is usually not associated with periodontal disease. This disease damages the teeth, gum, and jawbone of more than 80 percent of Americans by age 45.
Our emphasis is on early detection and prevention!
PERIODONTAL CARE
 Why do some patients have problems with periodontal infection and others seem not to? Gum disease is known to be hereditary, so this means the body defense against periodontal infection is impaired.
Why do some patients have problems with periodontal infection and others seem not to? Gum disease is known to be hereditary, so this means the body defense against periodontal infection is impaired.
Periodontal treatment is necessary when chronic infection conditions affect the health of your gums and damage the surrounding bone holding your teeth in place. Retaining your teeth is directly dependent on proper periodontal interventional care and professional regular maintenance follow-up.
Healthy gums enhance the appearance of your teeth, like a frame around a beautiful painting.
THE MOUTH AND BODY CONNECTION
Heart Disease
 Several theories exist to explain the link between periodontal disease and heart disease. One theory is that oral bacteria can affect the heart when they enter the blood stream, attaching to fatty plaques in the coronary arteries due to the buildup of fatty proteins. Blood clots can obstruct normal blood flow, restricting the amount of nutrients and oxygen required for the heart to function properly. This may lead to heart attacks.
Several theories exist to explain the link between periodontal disease and heart disease. One theory is that oral bacteria can affect the heart when they enter the blood stream, attaching to fatty plaques in the coronary arteries due to the buildup of fatty proteins. Blood clots can obstruct normal blood flow, restricting the amount of nutrients and oxygen required for the heart to function properly. This may lead to heart attacks.
Another possibility is that the inflammation caused by periodontal disease increases plaque build up, which may contribute to swelling of the arteries. Researchers have found that people with periodontal disease are almost twice as likely to suffer from coronary artery disease as those without periodontal disease. Periodontal disease can also exacerbate existing heart conditions. Patients at risk for endocarditis may require antibiotics prior to dental procedures. Your dentist and cardiologist will be able to determine if your heart condition requires use of antibiotics prior to dental procedures.
Stroke And Periodontal Disease
 Additional studies have pointed to a relationship between periodontal disease and stroke. In one study that looked at the causal relationship of oral infection as a risk factor for stroke, people diagnosed with acute cerebrovascular ischemia were found more likely to have an oral infection when compared to those in the control group.
Additional studies have pointed to a relationship between periodontal disease and stroke. In one study that looked at the causal relationship of oral infection as a risk factor for stroke, people diagnosed with acute cerebrovascular ischemia were found more likely to have an oral infection when compared to those in the control group.
Further research has shown that periodontal disease is directly related to the incidence of strokes.
Diabetes And Periodontal Disease
People with diabetes are more likely to have periodontal disease than people without diabetes, probably because diabetics are more susceptible to contracting infections. Those people who don’t have their diabetes under control are especially at risk.
Uncontrolled Type 2 diabetes patients are more likely to develop periodontal disease than those who are well-controlled. This means that the relationship with periodontal disease goes both ways – periodontal disease may make it more difficult for people who have diabetes to control their blood sugar.
Severe periodontal disease can increase blood sugar, contributing to increased periods of time when the body functions with high blood sugar. This puts diabetics at increased risk for complications. Thus, diabetics who have periodontal disease should be treated to eliminate the periodontal infection.
Kidney Disease And Periodontal Disease
Periodontal disease adversely affects the survival of patients with end-stage renal disease.
Lung Disease And Periodontal Disease
Respiratory Diseases
 Bacterial respiratory infections are acquired through aspiration (inhaling) of fine droplets from the mouth and throat into the lungs. These droplets contain germs that can breed and multiply within the lungs to cause damage. Bacteria found in the throat, as well as bacteria found in the mouth, can be drawn into the lower respiratory tract. This can cause infections or worsen existing lung conditions. People with respiratory diseases, such as chronic obstructive pulmonary disease, typically suffer from reduced protective systems, making it difficult to eliminate bacteria from the lungs.
Bacterial respiratory infections are acquired through aspiration (inhaling) of fine droplets from the mouth and throat into the lungs. These droplets contain germs that can breed and multiply within the lungs to cause damage. Bacteria found in the throat, as well as bacteria found in the mouth, can be drawn into the lower respiratory tract. This can cause infections or worsen existing lung conditions. People with respiratory diseases, such as chronic obstructive pulmonary disease, typically suffer from reduced protective systems, making it difficult to eliminate bacteria from the lungs.
Scientists have found that bacteria that grow in the oral cavity can be aspirated into the lungs to cause respiratory diseases such as pneumonia, especially in people with periodontal disease. This discovery leads researchers to believe that these respiratory bacteria can travel from the oral cavity into the lungs to cause infection.
Chronic Obstructive Pulmonary Disease (COPD) causes persistent obstruction of the airways. The main cause of this disease is thought to be long-term smoking. Chemicals from smoke or air pollution irritate the airways to cause obstruction. Further damage to the tissue and working function of the lungs can be prevented, but already damaged tissue cannot be restored – untreated or undetected COPD can result in irreversible damage. Bacteria can cause frequent bouts of infection in patients with COPD. Studies are now in progress to learn to what extent oral hygiene and periodontal disease may be associated with more frequent bouts of respiratory disease in COPD patients
Cancer
Research has found that men with a history of gum disease are 14 percent more likely to develop cancer than men with healthy gums. Specifically, men with periodontal disease may be 49 percent more likely than women to develop kidney cancer, 54 percent more likely to develop pancreatic cancer, and 30 percent more likely to develop blood cancers.
Osteoporosis
 Researchers have suggested that a link between osteoporosis and bone loss in the jaw. Studies suggest that osteoporosis may lead to tooth loss because the density of the bone that supports the teeth may be decreased, which means the teeth no longer have a solid foundation.
Researchers have suggested that a link between osteoporosis and bone loss in the jaw. Studies suggest that osteoporosis may lead to tooth loss because the density of the bone that supports the teeth may be decreased, which means the teeth no longer have a solid foundation.
